Emergency Pulmonology Clinic
Department for Intensive Care and Intoxications - Level 3
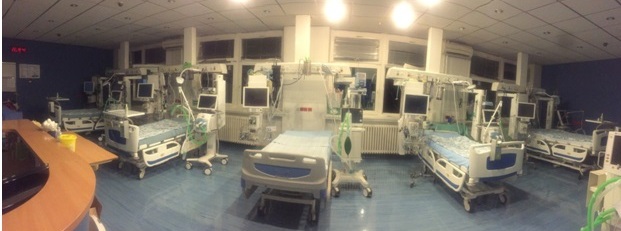
The Department for Intensive Care and Intoxications –level III (Intensive Care Unit - ICU) is a part of Emergency Pulmonology Clinic treating critically ill patients with a dysfunction of one or more organ systems, predominantly the respiratory or cardiovascular ones.
The Department has five patient beds provided with ventilation support, noninvasive and invasive haemodynamic monitoring (blood pressure, cardiac frequency, saturation, respiration count, diuresis, body temperature). Additional routinely used equipment includes a portable echocardiography device, bronchoscope, and instruments for continual renal function substitution.
Department physicians are engaged in the Unit for Invasive Diagnostics and Treatment intended for invasive haemodynamic procedures (right heart catheterisation, pericardiocentesis, placement of ports, cava filters, cava stents, ECMO and ECOS catheters, thromboaspirations, pulmonary angiography, balloon pulmonary agioplastica, embolisation of pulmonary arteries).
The Department employs six physicians – three specialists (Assist. Prof. Jovan Matijasevic, MD. PhD, Uros Batranovic, Srdjan Gavrilovic, MD), and three physicians specialising in Internal Medicine (Vladimir Carapic, Svetislava Milic, and Ana Andrijevic), as well as 21 nurses/medical technicians. The physicians of the Department are members of the Serbian Society of Intensive Care Medicine and the European Society of Critical Care Practitioners. They went for advanced training to the States (Mayo Clinic, Rochester), to Italy and other countries. Experienced in participating in clinical trials and international projects, they are also included in the global project iCertain, involving 40 countries from all over the world, leaded by the Mayo Clinic, while the Institute for Pulmonary Diseases of Vojvodina is a coordination centre.
The Head of the Department for Intensive Care and Intoxication is Assist. Prof. Jovan Matijasevic, MD. PhD, a Specialist in Internal Medicine, and the Head Nurse is Maja Stanojevic, a graduate health care organiser.
Intensive Care Department – Level 2
The Intensive Care Department - Level 2 is a modern respiratory unit of the Emergency Pulmonology Clinic the Institute designed in compliance with recommendations of the European Society of Critical Care Practitioners. The Department has five patient beds provided with equipment for noninvasive and invasive monitoring of vital parameters, and two beds for patients with multiresistant agents of their disease requiring isolation measures to be undertaken. The Department provides treatment for critically ill pulmonary patients, in compliance with the good clinical practice of the critical care medicine.
The Department is technically equipped in compliance with European standards, providing a continual monitoring of vital parameters, including a patient’s haemodynamic profile. Noninvasive ventilation adjusted to indications and the Protocol of the European Respiratory Society is carried out at the Department.
The staff of the Intensive Care Department – Level 2 includes its Head Assist. Prof. Dusanka Obradovic; an internist-pulmonologist, and current Chief of the Internal Medicine Department of the Medical Faculty of Novi Sad, Biljana Joves, MD. PhD, an internist, Ivana Vujovic, a clinical physician, and Jelena Repic, the Head Nurse.
Department for Pulmonary Thromboembolism
The Department for Pulmonary Thromboembolism provides treatment for patients with pulmonary embolism (PE) and deep venous thrombosis (DVT). As soon as a patient is clinically examined and assessed for a potential presence of PE and DVT, diagnostic procedures are undertaken including X-ray of the lungs, blood gas analyses, ECG, echocardiography, D-dimer test, coagulation, enzyme and biochemistry status evaluation. If the obtained test findings suggest PE may be involved, the definite diagnosis is established by CTPA – computerised angiography and perfusion scintigraphy of the lungs. Concurrently with diagnosing pulmonary thromboembolism, it is attempted to detect the thrombus site of origin applying ultrasonography of the lower extremity veins. If the thrombus origin is defined, a vascular surgery or a vena cava filter insertion are considered by a vascular surgeon in order to prevent pulmonary thromboembolism to reoccur.
Once the suspected pulmonary thromboembolism is confirmed by basic diagnostic tests, the treatment is initiated, depending on the severity of pulmonary thromboembolism. Massive pulmonary thromboembolism is treated by fibrinolytic therapy, monitoring a patient in the Intensive Care Unit of the Emergency Pulmonary Clinic. Stabilised patients and those with non- massive PE receive anticoagulation therapy (unfractionated and low-molecular heparin. Afterwards, the patients are translated to oral anticoagulation therapy, controlling their prothrombin time. Once the therapeutic effect is achieved, further controls are performed in the Thrombosis Prevention Unit in the Policlinic of the Institute, seven to ten days after the discharge from hospital and during the first month, and afterwards, as the therapy has been well regulated, once in a month. When new oral anticoagulant drugs are not contraindicated, they are introduced in the treatment, thus reducing the hospital treatment length, performing controls in three-month intervals. In case the thrombus resolution is not achieved after the applied treatment, chronic pulmonary hypertension develops due to pulmonary thromboembolism. This condition is assessed 3-6 months following acute PE (by echocardiography, right heart catheterisation, CTPA and perfusion scintigraphy). Based on the obtained findings, endarterectomy is indicated, representing a golden standard in CTEPH management, in case major branches of the pulmonary artery are obstructed, or balloon angioplasty in case peripheral branches are occluded. The latter procedures are performed in specialised centres selected by the International CTEPH Association.
As venous thromboembolism develops as a complication of other diseases, surgeries, traumas, infections, malignancies, thrombophilia, there is a close cooperation with other clinics of the Institute and the Clinical Centre of Novi Sad, as well as with the Service for Haemostasis and Thrombosis.
The Head of the Department is Jadranka Vucicevic-Trobok, MD, a Subspecialist in Pulmonology.
Associates: Sandra Pekovic, MD, a Subspecialist in Pulmonology, Stanislava Sovilj-Gmizic, a Specialist in Internal Medicine, Milica Miric, MD, specializing in Internal Medicine.
Department for Pulmonary Hypertension and Chronic Pulmonary Heart
As an integral part of the Clinic for Emergency Pulmonology, this department is intended for emergency treatment of patients with acute/chronic respiratory failure usually due to chronic obstructive pulmonary disease (COPD), right heart decompensation, or a combined cardiorespiratory disease. These patients usually require a noninvasive mechanical ventilation in addition to other medicamentous and supportive treatment. The diagnosis and treatment of the underlying cause of the disease are further steps in patients admitted to intensive and semi intensive units and transferred to the clinical department for further treatment.
Over the last five-year period, patients with primary pulmonary hypertension (PAH) have been separately diagnosed and treated in the Department, complying to international guidelines and in cooperation with other centres in the country and abroad (the Clinical Centre of Serbia in Belgrade and AKH Clinic in Vienna). Most diagnostic procedures can be carried out in a short period of time, including the right heart catheterisation, which is a golden standard, and is carried out in the intensive care unit.
As a single referral centre for PAH in Vojvodina, due to persistent efforts and in cooperation with the Ministry of Health, we have succeeded to provide a part of the latest, specific PAH treatment for these patients. At present, two groups of drugs are available: receptor 5 phosphodiesterase inhibitors (sildenafil), and endolenyn receptor 1 antagonist (bosentan); additional combinations are also available in clinical trials with selected patients. Each drug administration is approved the Board for Pulmonary Hypertension, presided by prof. Ilija Andrijevic, MD. PhD.
Head of the Department: Prof. Ilija Andrijevic, MD. PhD.
Physicians: Stoja Krunic, MD, a Specialist in Pulmonology, Senka Milutinov, MD. PhD, a Specialist in Pulmonology